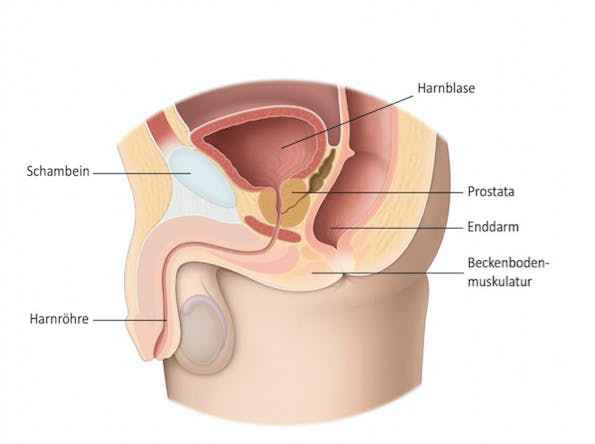
Yes, men have a pelvic floor! Although pelvic floor training, especially in relation to childbirth and pregnancy, is familiar to almost every woman, this topic is still a taboo topic for men. Through targeted exercises of the pelvic floor, a steady loss of urine can be regulated. An erectile dysfunction can also be treated with the help of physiotherapy.
Difference between men and women
The pelvic floor closes the abdominal cavity downwards and is formed by three muscle layers. It mainly serves to secure the position of the abdominal and sexual organs. It can be controlled to a large extent and can therefore be trained like any other skeletal muscle. The pelvic floor of a man differs from that of a woman: it is anatomically more stable, is made of denser muscle tissue and has to withstand a wide range of stresses. The male urethra is much longer and has a natural barrier to the prostate.
The symptoms can range from nycturia (frequent urination at night), polakisuria (too frequent urination in small amounts), dysuria (difficult urination), increased urination to urine loss during sports. A weakened or missing erection is also an issue in therapy.
Incontinence occurs primarily after prostate, bladder and bowel surgery or during radiation of prostate cancer. Other possible causes of incontinence include trauma, organic problems such as heart failure, bladder stones or diabetes mellitus, and neurological diagnoses such as stroke.
Before and after prostate surgery
Physiotherapeutic treatment is strongly recommended for the above-mentioned complaints as well as before and after prostate surgery. Depending on the symptoms, a diagnosis is made at the beginning of the therapy. Patient and therapist work together on the success of the therapy. Everyday tips, relaxation techniques, breathing and posture training as well as potency counselling are discussed during the therapy. Functional abdominal muscle training and swelling training as well as strengthening of the urethral sphincter are also initially done together. This requires personal initiative. The patient can make a significant contribution to the success of the therapy. In addition, the therapist uses passive techniques such as lymph drainage, pelvic mobilisation, taping and electrotherapy.
